The New York Times has confirmed that at least 88 candidates are under active preclinical investigation in laboratories across the world, with 67 of them slated to begin clinical trials before the end of 2021.
Those trials may begin after millions of people have already received the first wave of vaccines. It will take months to see if any of them are safe and effective. Nevertheless, the scientists developing them say their designs may be able to prompt more powerful immune responses, or be much cheaper to produce, or both — making them the slow and steady winners of the race against the coronavirus.
“The first vaccines may not be the most effective,” said Ted Ross, the director of the Center for Vaccines and Immunology at the University of Georgia, who is working on an experimental vaccine he hopes to put into clinical trials in 2021.
Many of the vaccines at the front of the pack today try to teach the body the same basic lesson. They deliver a protein that covers the surface of the coronavirus, called spike, which appears to prompt the immune system to make antibodies to fight it off.
But some researchers worry that we may be pinning too many hopes on a strategy that has not been proved to work. “It would be a shame to put all our eggs in the same basket,” said David Veesler, a virologist at the University of Washington.
In March, Dr. Veesler and his colleagues designed a vaccine that consists of millions of nanoparticles, each one studded with 60 copies of the tip of the spike protein, rather than the entire thing. The researchers thought these bundles of tips might pack a stronger immunological punch.
When the researchers injected these nanoparticles into mice, the animals responded with a flood of antibodies to the coronavirus — much more than produced by a vaccine containing the entire spike. When the scientists exposed vaccinated mice to the coronavirus, they found that it completely protected them from infection.
The researchers shared their initial results this month in a paper that has yet to be published in a scientific journal. Icosavax, a start-up company co-founded by Dr. Veesler’s collaborator, Neil King, is preparing to begin clinical trials of the nanoparticle vaccine by the end of this year.
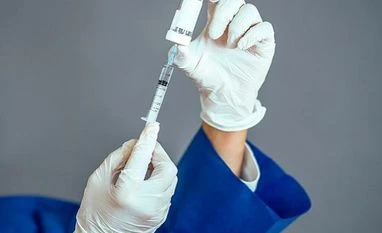
ImageResearch at a lab of the French vaccine maker Valneva, which is taking a conventional approach to developing a vaccine, using viruses that are inactivated by chemicals.
Antibodies are only one weapon in the immune arsenal. Blood cells known as T cells can fight infections by attacking other cells that have been infiltrated by the virus.
“We still don’t know which kind of immune response will be important for protection,” said Luciana Leite, a vaccine researcher at Instituto Butantan in São Paulo, Brazil.
It’s possible that vaccines that arouse only antibody responses will fail in the long run. Dr. Leite and other researchers are testing vaccines made of several parts of the coronavirus to see if they can coax T cells to fight it off.
“It’s a second line of defense that might work better than antibodies,” said Anne De Groot, the C.E.O. of Epivax, a company based in Providence, R.I.
Epivax has created an experimental vaccine with several pieces of the spike protein, as well as other viral proteins, which it plans to test in a clinical trial in December.
The effectiveness of a vaccine can also be influenced by how it gets into our body. All of the first-wave vaccines now in clinical trials have to be injected into muscle. A nasal spray vaccine — similar to FluMist for influenza — might work better, since the coronavirus invades our bodies through the airway.
)