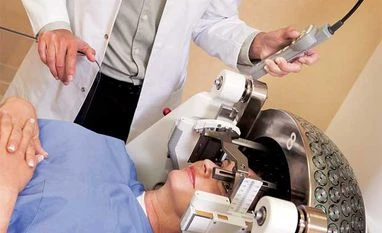
A brain scan may predict alzheimer's disease. Should you get one?
Some experts fear PET scans offer few benefits, at substantial costs
)
premium
3 min read Last Updated : Aug 03 2019 | 10:56 PM IST
Juli Engel was delighted when a neurologist recommended a PET scan to determine whether amyloid — the protein clumps associated with an increased risk of Alzheimer’s disease — was accumulating in her mother’s brain.
“My internal response was, ‘Yay!’” said Engel, 65, a geriatric care manager in Austin, Tex., who has been making almost monthly trips to help her mother in Florida. “He’s using every tool to try to determine what’s going on.”
Sue Engel, who’s 83 and lives in a retirement community in Leesburg, Fla., has been experiencing memory problems and other signs of cognitive decline for several years. Her daughter checked off the warning signs: her mother has been financially exploited, suffered an insurance scam, caused an auto accident.
Medicare officials decided in 2013, shortly after PET (positron emission tomography) amyloid imaging became available, that they lacked evidence of its health benefits. So outside of research trials, Medicare doesn’t cover the scans’ substantial costs ($5,000 to $7,000, the Alzheimer’s Association says); private insurers don’t, either.
Juli Engel thinks Medicare should reimburse for the scan, but “if necessary, we’ll pay for it out of pocket,” she said.
Her mother already has an Alzheimer’s diagnosis and is taking a commonly prescribed dementia drug. So she probably doesn’t meet the criteria developed by the Alzheimer’s Association and nuclear medicine experts, which call for PET scans only in cases of unexplained or unusual symptoms and unclear diagnoses.
But as evidence mounts that brain damage from Alzheimer’s begins years before people develop symptoms, worried patients and their families may start turning to PET scans to learn if they have this biomarker.
They have few alternatives. Scientists at Washington University in St. Louis announced on Thursday that they’ve developed a blood test for amyloid that can predict the development of plaques in the brain, but it is years away from use in doctors’ offices.
Some experts fear PET scans offer few benefits, at substantial costs. “There are lots of incentives, including financial incentives, for doing more testing and interventions,” said Dr. Kenneth Langa, a researcher at the University of Michigan and author of a recent article in JAMA Internal Medicine about diagnosis of early Alzheimer’s disease. “My hope is we’ll think hard about the unintended downsides.”
What downsides? Amyloid plaques occur commonly in older people’s brains, but not everyone with amyloid will develop dementia, which probably involves multiple factors. Nor does a negative PET scan mean someone won’t develop dementia.
Biostaticians at the University of California, Los Angeles, have calculated that a 75-year-old man with amyloid has a 17.2 percent lifetime risk of developing Alzheimer’s dementia; for a woman that age, with a longer life expectancy, the figure is about 24 percent.
That’s primarily because Alzheimer’s rates climb steeply at older ages, when people grow more likely to die of other causes before they can develop symptoms. (With additional biomarkers, or with the condition called mild cognitive impairment, the lifetime risk rises.)
But older people may also be among the 30 percent or so of those with amyloid deposits who, for unexplained reasons, retain normal cognition.
“If we start treating everyone with preclinical Alzheimer’s, we’ll treat a lot of people who would never have gone on to have dementia at all,” Dr. Langa said.
Moreover, what treatments would those be? Multiple trials have failed to find drugs that prevent, reverse or slow Alzheimer’s disease, perhaps because these treatments were introduced too late in the disease’s course.
©2019 The New York Times News Service
Topics : Alzheimer’s
