Her infant, Tejash, is one of more than a 100 children who have died at a government hospital in Kota in the state of Rajasthan since early December.
Infant deaths are common in India, but the spike in fatalities at a state-run institution and evidence of poor hygiene, broken equipment and staff shortages has made headlines and triggered a row between the two main political parties.
District data in fact shows the infant mortality rate at the JK Lon Hospital in Kota has improved to 5.69 per cent with 963 deaths in 2019 down from 6.11 per cent in 2018, when 1,005 deaths were reported.
But details from affected families and two preliminary investigations have emerged, embarrassing the regional government and local health authorities.
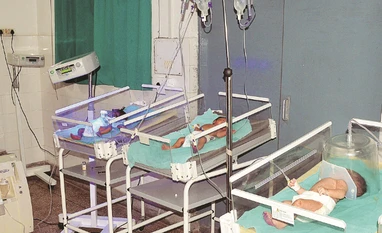
Padma said there were three or four infants in each bed when she was there in late December.
“Why are you crying? Your child is going to die anyway,” Padma recalled one doctor telling her, as she sat weeping beside her husband, Sanjay, and daughters — Kanika, 6, and Purvi, 4.
Reuters spoke with the parents of nine children who either died or were being treated at the hospital. All described staff shortages, poor sanitary conditions and a lack of basic provisions such as blankets despite very cold weather.
Rajasthan Health Minister Raghu Sharma tweeted that most of the infants who died had low birth weights and were in critical condition. He vowed “strict action” would be taken against any officials found guilty of negligence.
At least 112 children have died at the hospital since the start of December, even as authorities scrambled to bring in additional staff and equipment amid public outcry.
Around three quarters of the recent deaths occurred in JK Lon’s neo-natal intensive care unit (NICU), which treats babies up to a month old, said an official directly aware of the matter.
Hospital officials said infant mortality rates may appear high, partly because it handles many referral cases and is a hospital of last resort. It is the only one with an NICU in a 200 km radius.
Shubham Hada, who lost his two-day-old son at the hospital to what he was told was a severe infection, said: “Parents had to monitor their babies all night by themselves in the NICU. There were no doctors after 10 pm, when the shift changed.”
Pooja, holding her sick 2-month-old infant in her lap, said authorities distributed blankets and room heaters only late last week, despite a severe cold wave across northern India since late December.
)

